Walk into any drugstore in America and you can buy DHEA in a 25 mg capsule next to the magnesium. Walk into most primary-care offices and you can sit through an hour-long appointment without it being mentioned once. That gap — between a hormone you can buy off a shelf and a hormone that almost no one is testing — is where this story begins.
What DHEA Is (and Isn’t)
DHEA is short for dehydroepiandrosterone, a 19-carbon steroid hormone produced primarily by the zona reticularis of your adrenal cortex. A smaller amount is secreted by the ovaries (in women) and the testes (in men), and trace amounts originate in the brain itself. By volume, DHEA and its sulfated form DHEA-S together make up the most abundant circulating steroid hormones in healthy adults — outstripping cortisol, testosterone, and estradiol combined.
It is, biochemically speaking, a precursor. Cells throughout your body — in muscle, fat, brain, vaginal tissue, skin, breast — pick up DHEA from the bloodstream and convert it locally into whichever downstream hormones the tissue is equipped to make. In one woman’s vulvar tissue, DHEA might be converted into estradiol; in another woman’s sebaceous gland, into testosterone and then dihydrotestosterone. The same molecule, very different outcomes.
This local-conversion property is what endocrinologists call intracrinology: instead of the adrenals and gonads doing all the hormone-making and shipping the finished product to the rest of the body, DHEA acts like a pre-cut raw material that tissues finish on demand. The implication is profound — it means circulating DHEA-S is one of the few hormones the body can dial up or down in a tissue-specific way without flooding the whole system.
DHEA vs DHEA-S: Why Labs Measure One and Not the Other
“DHEA” and “DHEA-S” are not the same molecule, and this trips up almost every woman who tries to interpret her own lab work. DHEA is the unconjugated, biologically active form. DHEA-S is DHEA with a sulfate group attached — a process performed mostly in the adrenal glands by an enzyme called SULT2A1. The sulfated form is largely inactive on its own, but it acts as a stable reservoir: tissues remove the sulfate when they want to use the hormone.
The reason commercial labs almost always order DHEA sulfate rather than free DHEA is purely practical. DHEA itself has a half-life of about 30 minutes and fluctuates significantly throughout the day. DHEA-S has a half-life closer to 12 hours, circulates at far higher concentrations, and gives a clean snapshot of average adrenal output. If you have ever asked your doctor for a “DHEA blood test,” what got drawn was almost certainly DHEA-S.
The DHEA Decline: Why Your Levels Crash With Age
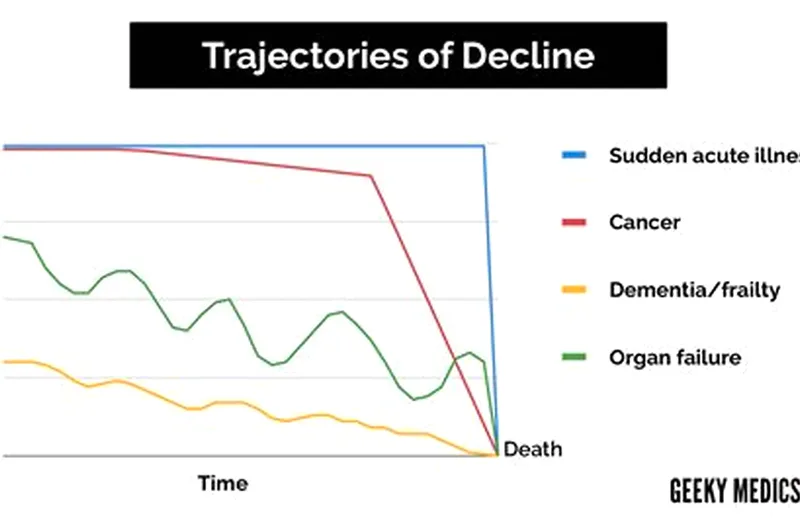
DHEA-S concentrations peak in the mid-20s, then begin a steep, lifelong descent that is more dramatic than the decline of any other steroid hormone. By age 50, the average woman has roughly 30–40% of her peak DHEA-S. By age 70, that number is closer to 10–20%. This trajectory is so reliable across populations that some researchers refer to it as adrenopause.
The drop is not caused by ovarian failure — DHEA is primarily adrenal. It is also distinct from cortisol, which holds steady or even rises with age. What you’re looking at when you look at a DHEA-S decline curve is the slow regression of a specific zone of the adrenal cortex, the zona reticularis, which preferentially atrophies as we age.
The clinical question this raises has been debated for forty years: does replacing DHEA back to youthful levels produce meaningful benefits? The honest answer, in 2026, is “in some populations, modestly, for some endpoints — yes; for most healthy women with intact adrenal function, probably not enough to justify long-term unsupervised supplementation.”
What DHEA Actually Does in the Female Body
The honest answer is: it does whatever the local tissue tells it to do. But here is a tour of the systems where the evidence is most developed.
Sexual and vaginal health
The strongest, FDA-cleared clinical signal for DHEA in women is local. Vaginal Prasterone (Intrarosa), inserted nightly, converts in the vulvovaginal epithelium into estrogens and androgens, reversing the thinning, dryness, and pain that come with menopausal atrophy. This is now a standard option for postmenopausal women with painful intercourse who cannot or prefer not to use vaginal estradiol.
Energy and adrenal function
In women with documented adrenal insufficiency (Addison’s disease, hypopituitarism), oral DHEA replacement of 25–50 mg/day has shown improvements in mood, energy, and quality-of-life scores in multiple randomized trials. In women with normal adrenal function, results are far less consistent — there is no meta-analytic signal that boosting an already-normal DHEA level produces measurable energy gains.
Libido
Mixed but real. Women with hypoactive sexual desire disorder, particularly post-menopause, show modest improvements in subjective desire and arousal at doses of 25–50 mg/day in some trials. The effect is not dramatic and is concentrated in women who started with low baseline DHEA-S.
Skin and aging
Local production of estrogens and androgens in skin influences sebum, collagen, and elasticity. DHEA may improve skin hydration and reduce some markers of aging, but the effect size in well-controlled trials is small.
Bone density
DHEA appears to support bone mineral density indirectly via its conversion to estrogens. The effect is modest and unlikely to replace established osteoporosis therapy, but in women with both low DHEA-S and low bone density, replacement may contribute additional benefit.
Mood and cognition
Several trials in midlife and postmenopausal women have shown modest improvements in depressed mood scores with DHEA replacement. Cognitive effects are inconsistent.
Symptoms of Low DHEA in Women
Low DHEA-S does not present with a tidy syndrome the way hypothyroidism does. It tends to show up as a constellation of vague but real complaints — most of which are also caused by ten other things, which is precisely why clinicians who don’t test DHEA-S miss it constantly.
- Persistent fatigue that doesn’t resolve with sleep
- Reduced libido and difficulty achieving arousal
- Dry skin and reduced skin elasticity
- Low mood and reduced sense of vitality
- Slow recovery from physical or psychological stress
- Decreased muscle strength relative to age-matched peers
- Vaginal dryness, especially in perimenopausal women
- Reduced bone density on DEXA
None of these are specific. All of them warrant testing rather than guessing — and crucially, they warrant testing alongside estradiol, total/free testosterone, FSH, thyroid panel, and cortisol, because the DHEA-S number alone tells you almost nothing in isolation. See our deep-dive on DHEA-S testing and on interpreting low and high DHEA results.
Why Take DHEA at Night? (Spoiler: You Probably Shouldn’t)
Search interest in “why take DHEA at night” spikes every January. The short answer: most endocrinologists explicitly advise against it. The body’s natural DHEA production peaks in the early morning hours as part of the circadian rhythm that also drives cortisol release. Mimicking that timing — taking oral DHEA with breakfast — gives you the smoothest pharmacokinetic profile and the lowest risk of sleep disruption.
Evening dosing has gained popularity through one particular pocket of online wellness culture that argues nighttime DHEA supports overnight repair. The evidence for this is essentially nonexistent, while reports of insomnia, vivid dreams, and elevated heart rate at night are extremely common in clinical practice. If your DHEA dose is making it hard to sleep, the first move is to shift it to morning, not to add melatonin on top.
OTC DHEA Supplements: The Unregulated Wild West
This is the section the supplement industry would prefer you skipped. In the United States, DHEA is regulated as a dietary supplement under the Dietary Supplement Health and Education Act of 1994 (DSHEA). What that classification actually means in practice:
- The FDA does not verify what is in the bottle before it goes on sale.
- Manufacturers are responsible for testing their own products; oversight is mostly post-market.
- “Structure-function” claims (e.g., “supports healthy aging”) require no clinical evidence.
- Independent testing organizations — ConsumerLab, NSF International, USP — routinely find products that test at 50%, 150%, or in a few documented cases more than 200% of the labeled dose.
- Acceptable claims on the label say almost nothing about purity, contaminants, or batch consistency.
The practical fallout: a woman who tracks a 25 mg dose religiously, sees a clinical change, and then switches brands may be unknowingly doubling or zeroing-out her actual hormone exposure. There is no pre-market control to prevent this. Choosing a USP- or NSF-certified product narrows the variance somewhat, but it does not eliminate it.
This is the core argument against treating OTC DHEA the way you would treat a multivitamin. DHEA is a hormone. Inconsistent hormone dosing produces inconsistent endocrine effects. Our supplement buyer’s guide walks through what to actually look for on a label if you are going to buy OTC anyway.
Side-by-side
OTC DHEA Supplements vs. Prescription DHEA Therapy
The same hormone, two completely different regulatory and clinical realities. This is the picture the supplement industry doesn’t put on the bottle.
| What you get | OTC supplement | Prescription / supervised |
|---|---|---|
| Regulatory oversight | FDA does not pre-approve content or purity | FDA-evaluated for purity, potency, and indication |
| Form availability | Capsules, sublingual tablets, topical creams | Vaginal insert (Prasterone), compounded topical, compounded oral |
| Dose precision | Independent labs find ±30–50% deviation from label | Pharmacy-compounded or branded — verified content |
| Lab work | Self-directed; usually none | DHEA-S, estradiol, total/free testosterone before and after |
| Clinician oversight | None required | Licensed prescriber; re-test at 90 days |
| Indication | Marketed for energy, libido, “anti-aging” — claims unregulated | Approved for menopausal dyspareunia (Intrarosa); off-label for adrenal-insufficiency support |
| Realistic cost (monthly) | $8–$40 per bottle | $30–$220 depending on form and insurance |
Prescription DHEA: When OTC Isn’t Enough
There are exactly two prescription pathways for DHEA in the United States in 2026:
1. Vaginal Prasterone (Intrarosa)
FDA-approved in November 2016 for moderate-to-severe dyspareunia due to menopause. A 6.5 mg suppository inserted nightly converts locally in the vaginal tissue into estrogens and androgens, restoring epithelial thickness without raising systemic estradiol significantly. This is the cleanest, most evidence-backed DHEA application in clinical medicine. See our full review of vaginal DHEA.
2. Compounded oral or topical DHEA
Some licensed compounding pharmacies dispense pharmaceutical-grade DHEA in custom doses (often 5–25 mg oral capsules, or transdermal creams of varying strength) on a clinician’s prescription. This is the route most commonly used for women with documented adrenal insufficiency and for off-label use in menopausal symptom management. Compounded DHEA is held to higher quality standards than retail supplements but is more expensive and requires an active provider relationship.
The Modern Path: Personalized Hormone Care
For decades, women’s hormone health in the United States looked like this: a 7-minute appointment with an obstetrician-gynecologist who was trained in delivering babies, not in adrenal physiology; a vague reassurance that levels were “within range”; a prescription for an SSRI; and the rest of the work done by the woman herself, alone, on the internet.
What changed over the last five years is the rise of telehealth practices that specialize specifically in hormone optimization — staffed by clinicians with NAMS (North American Menopause Society) or anti-aging fellowship training, ordering comprehensive panels rather than a single TSH, and re-testing at intervals instead of writing one-and-done prescriptions.
What this looks like in practice:
- A 10–15 minute structured intake that documents your symptoms, history, current supplements, and goals.
- A comprehensive lab order — DHEA-S, free and total testosterone, estradiol, FSH, LH, thyroid panel, cortisol, often a metabolic panel.
- A 30–45 minute video consultation with a licensed clinician who reads your numbers in context.
- A plan that may include prescription Prasterone, compounded DHEA, an estradiol protocol, a testosterone protocol — or, frequently, no DHEA at all, because the numbers don’t support it.
- A 90-day follow-up with retesting before any prescription is continued.
The point is not that telehealth is magic. The point is that this is the first time in two generations that the standard-of-care for hormone-curious women has caught up to what the literature actually supports.